An interesting article titled “Percutaneous exposure incidents: a review of practice and awareness of current protocols at a Dental Faculty” written by Siddiqi et al. appears in Oral Surgery in 2017 (vol. 10, e80-e87). The article discusses accidental exposure to blood-borne pathogens at the dental office. In the past the possibility of this occurring has been discussed on this site see for example the posts More Dental Patients Warned of Potential HIV and Hepatitis Exposure in Pennsylvania and Infection Control Lapse in Hawaii at VA Dental Clinic.
Sharps and needlestick injuries are sources of infections with blood-borne pathogens (such as Hepatitis B, Hepatitis C, and HIV) in dentistry and are referred to broadly as a percutaneous exposure incident. The authors state:
“The intimate nature of the patient-dentist environment, the presence of blood and saliva, the routine use of sharp instruments, and the frequent creation of aerosols combine to make the dentist’s workplace a potentially hazardous site for blood-borne viral infections.”
The authors state that the Centers for Disease Control and Prevention (CDC) and other studies suggest that as a result of a needlestick injury by a healthcare worker the risk of acquiring HIV is 0.3%, Hepatitis B is 45% and Hepatitis C is up to 10%. Non-reporting or under reporting a percutaneous exposure incident is very common among healthcare workers.
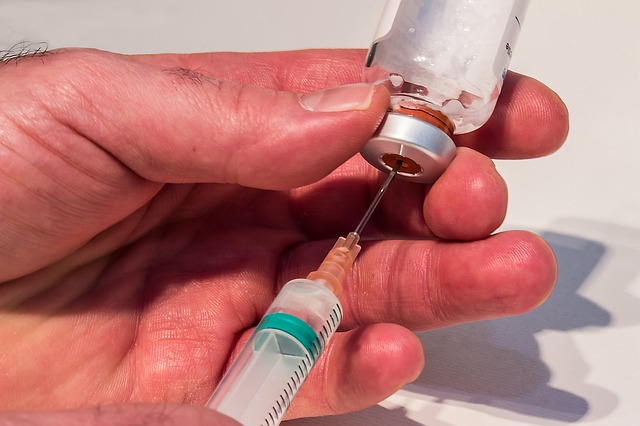
The authors conducted a survey of fourth and fifth year Bachelor of Dental Surgery, postgraduate students, and academic staff during 2012 and 2013 at the University of Otago in New Zealand. The questionnaire consisted of 23 open-ended and close-ended questions regarding questions related to needlestick injuries. A total of 234 surveys were completed with 61.2% of these surveys being answered by undergraduate students. Seventy respondents (29.9%) reported having seen a percutaneous injury during 2012 and 2013. Most of the exposures occurred (68.7%) among undergraduate dental students. The type of dental instrument most involved in a sharp or needlestick injury included a dental anesthetic needle in 31 cases (34.8%), a bur in 25 cases (28.1%) and scalar tip in 19 cases (21.3%). Fifty-one (76.1%) respondents stated the percutaneous injury occurred with a contaminated object. Twenty-two (32.8%) percutaneous injuries were not reported and around 35% of those who had injuries were not aware that the source patient had HIV or Hepatitis. The most common reasons that an injury with a sharp object occurred were lapses in concentration (31.3%), time constraints (14.1%), stress (14.1%) and fatigue (10.1%). Further just three (4.3%) respondents took a post-exposure prophylaxis after the percutaneous injury. A total of 182 of the 234 respondents (78.4%) were in favor of having additional education and training on needlestick injury prevention and management. The authors state
“Students need better training to minimise ‘culture of silence’, accidental needlestick and sharps injuries, which can have serious health, psychological, ethical and financial implications. Institutions (dental/medical) should not only reinforce the importance of properly reporting all PEIs [percutaneous exposure incidents] but should also go beyond the conventional teaching of universal procedures to minimi[z]e PEIs [percutaneous exposure incidents].”
The authors feel that improvements are needed to develop a culture that properly reports sharps and needlestick injuries and adopts post-exposure prophylaxis when needed. They feel that improvements can be made to dental education with respect to infection control and prevention measures. They do point out a few limitations of their study such as possible recall bias and untruthful answers given by the respondents to the survey questions.
